Table of Contents
Hormones Definition
Hormones are chemical messengers that are produced by endocrine glands and reach the bloodstream directly. Many hormones can be secreted by a single gland or cell, and multiple glands can produce the same hormone.
Types of Hormones
Hormones are divided into several categories.
1. Amine Hormones: Tyrosine-derived peptide hormones.
2. Thyroid Hormones: The thyroid gland is wrapped around the trachea in the lower neck. The two iodine-containing hormones thyroxine (T4) and triiodothyronine (T3) are secreted by follicles (T3). Thyroid hormones (TH) are hormones that control oxygen intake, growth, and brain development. T4 is secreted in greater quantities, but it is primarily converted to T3, which is the more active version.
3. Adrenal Medullary Hormones: There are two adrenal glands on top of each kidney.An inner adrenal medulla and a surrounding adrenal cortex make up each gland’s endocrine components. Catecholamines epinephrine (E) and norepinephrine (NE) are secreted by the medulla. These hormones have comparable effects on sympathetic nerves. There is more epinephrine secreted than norepinephrine.
4. Peptide Hormones: The bulk of hormones are made up of peptides. Larger preprohormones are produced first, then cleaved to prohormones in the ER. In the Golgi, the prohormone is converted to the active hormone. These hormones have the potential to act as neurotransmitters. Calcitonin is a peptide hormone produced by thyroid gland parafollicular cells that helps regulate blood Ca2+ levels.
5. Steroid Hormones: Steroid hormones are produced by the adrenal cortex and the gonads.
6. Adrenal Cortex Hormones: Aldosterone regulates the kidney’s processing of Na+, K+, and H+ ions, which helps to maintain mineral balance (mineralocorticoid). Cortisol and corticosterone influence glucose (glucocorticoid) and other organic substances metabolism. Stress reactions and immune system modulation are also influenced by cortisol. Adrenal androgens have a lower potency than testosterone, the other androgen. Play a function during puberty and in adult females.
7. Hormones of the Gonads: The main androgen produced by the testes is testosterone. Androgens are the source of the main female hormone, estradiol, which is produced by the ovaries.
Hormones Physiology
Hormone Transport in Blood: Water-soluble hormones are carried dissolved in the plasma, whilst others circulate attached to plasma proteins in the blood. To reach its target cells, the unbound hormone diffuses past capillary walls.
Hormone Metabolism and Excretion: The rate of production and clearance of a hormone determines its plasma concentration. Hormones are eliminated by the kidneys or processed in the blood or target cells.
Hormones Mechanism of Action
Hormones go through the bloodstream to all tissues, but only cells with receptors for the hormone operate as target cells. Up-regulation compensates for a low hormone concentration by increasing the number of receptors, and down-regulation compensates for a high hormone concentration by decreasing the number of receptors.
A hormone can limit the number of receptors available for a second hormone, lowering the second hormone’s efficacy (antagonism). A hormone can also increase the number of receptors for a second hormone, therefore boosting the efficacy of the latter (permissiveness).
Peptide hormone and catecholamine receptors are found on the plasma membrane’s extracellular surface, while steroid and thyroid hormone receptors are mostly found on the intracellular surface. Hormone receptor binding affects: (1) ion channels, (2) receptor-associated enzyme activity, (3) JAK kinase activity, and (4) G proteins and second messengers. Genes can also be activated or inhibited, affecting the rate at which proteins transcribed by these genes are synthesised.
Hormones Regulation
1. Regulate by plasma concentrations of certain substances: In a negative feedback loop, plasma concentrations of specific ions or nutrients may affect the secretion of a hormone, and the hormone, in turn, may control the concentration of its regulators.
2. Neuronal control: Some hormones may be controlled by the autonomic or central nervous systems.

3. Other hormones govern secretion: Hormones known as “tropical hormones” may regulate the release of other hormones.
4. Hypothalamic and pituitary control system: The pituitary gland (hypophysis) is located below the hypothalamus and is linked to it through the infundibulum.
Long-loop negative feedback occurs when the last hormone in a chain of regulation can exert negative feedback on the hypophysio-pituitary system. Short-loop negative feedback occurs when an anterior pituitary hormone has a negative feedback impact on the hypothalamus. Pituitary hormones that have no effect on other endocrine glands are detected.
Pituitary Gland
The pituitary gland consists of two lobes:
Posterior pituitary (neurohypophysis): A neuronal extension of the hypothalamus, the posterior pituitary (neurohypophysis). The hypothalamus produces posterior pituitary hormones, which are then stored in the posterior pituitary. The hormones (a) oxytocin promotes smooth muscle contraction in females’ breasts and uterus, and (b) vasopressin (antidiuretic hormone or ADH) contributes in water excretion control and blood pressure regulation.
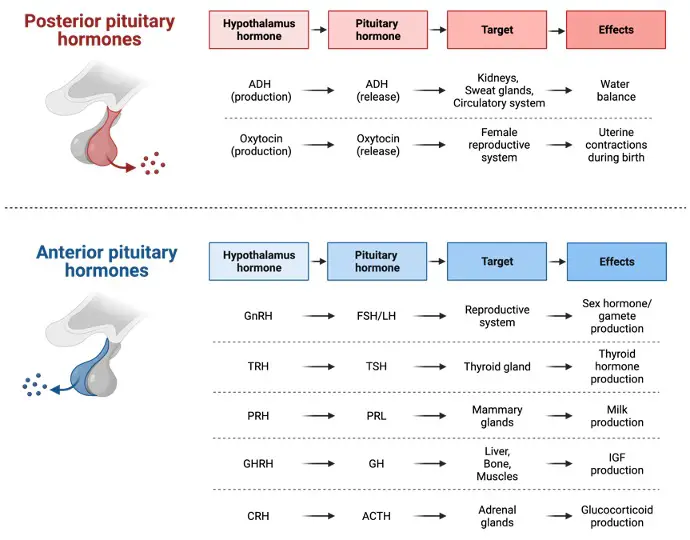
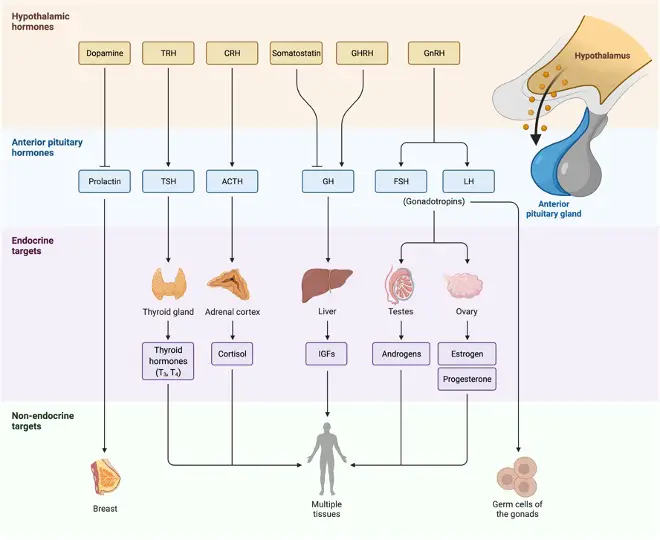
Anterior pituitary (adenohypophysis): Blood arteries termed hypothalamo-pituitary portal vessels connect the anterior pituitary to the hypothalamus. Hypophysiotropic hormones, which are produced in the hypothalamus, regulate the secretion of anterior pituitary hormones (all peptides), which in turn regulate the release of hormones from other endocrine glands. Such a control chain’s adaptive benefit is that it enables for more accurate feedback control.
Thyroid-stimulating hormone (TSH, thyrotropin) stimulates thyroid production of T4 and T3. The adrenal cortex secretes cortisol in response to a hormone called adrenocorticotropic hormone (ACTH). Follicle-stimulating hormone (FSH) and luteinizing hormone (LH) are gonadotropins that promote estradiol and progesterone production from the ovaries and testosterone secretion from the testes, as well as control ova and sperm growth and development.
Growth hormone (GH) stimulates the liver to produce insulin-like growth factor I (IGF-I), a growth hormone that has direct effects on metabolism. Prolactin does not regulate the release of other hormones, although it does increase the growth of mammary glands and milk production in females.
Hypophysiotropic Hormones
Neurons release these hormones in response to action potentials. The anterior pituitary hormone that each of these hormones regulates is named after it. Corticotropin-releasing hormone (CRH) stimulates ACTH synthesis (CRH). The growth hormone-releasing hormone (GHRH) promotes GH production. TSH or thyrotropin secretion is stimulated by thyrotropin-releasing hormone (TRH). The gonadotropin-releasing hormone (GnRH) increases gonadotropin secretion (FSH and LH). The hormone somatostatin (SS) suppresses GH production. Prolactin-inhibiting hormone (PIH) is a hormone that prevents prolactin from being secreted.
Candidate Hormones
Candidate hormones do not match the traditional definition of hormones for the following reasons:
- Their roles are unknown; for example, melatonin generated by the pineal gland is thought to have a role in circadian cycles and sleep.
- They operate as agents, but it is unknown whether they reach target cells via paracrine or autocrine blood, for example, growth factors.
Endocrine Hormones Disorders
1. Hyposecretion: Primary hyposecretion occurs when a gland produces too little hormone as a result of its inability to function correctly. A genetic deficit of an enzyme, a dietary shortage of a precursor, illness, and other factors might all play a role. Secondary hyposecretion occurs when a gland secretes too little hormone because there isn’t enough tropic hormone to activate it.
2. Hypersecretion: Primary hypersecretion occurs when a gland secretes too much hormone, whereas secondary hypersecretion occurs when a gland is overstimulated by its tropic hormone.
3. Hyporesponsiveness: A lack of receptors, a fault in the signal transduction pathway, or a lack of an enzyme that catalyses hormone activation prevents target cells from responding to the hormone. The insulin-target cells in diabetes mellitus are hyporesponsive to the hormone insulin.
4. Hyperresponsiveness: Thyroid hormone hypersecretion can cause hyperresponsiveness to epinephrine and, as a result, an increase in heart rate.







