What is Blood Group?
o Blood group is the classification of blood by the presence of specific antigen on the surface membrane of Red Blood cells (RBC). These antigens have resulted from the expression of allelic genes and linked genes.
o Antigens are molecules that evoke an immune response but some antigens are originated in our body so the immune system does not react to them.
o Antigens can be protein (e.g., Rh system) or sugar like glycoproteins or glycolipids (e.g., ABO system).
o The role of many of such antigens is still not clear however they are very important factors to be considered during blood transfusion because these antigens can evoke an immune response in the recipient body against non-self RBC antigen.
Blood Group Classification Systems
o Blood group systems are the group of antigens that is known to be controlled by a single gene or complex closely linked homologous genes.
o They are genetically distinct from each other.
o Genetic variations are identified for a blood group system along with its antigen, then sequenced and confirmed for the phenotype.
o As of 2021, a total of 43 blood group systems with 345 antigens are recognized by the International Society of Blood Transfusion (ISBT).
ABO Blood Group System
Some important Blood group systems are listed below;
In 1900, Karl Landsteiner observed RBCs agglutination in some individuals caused by transfusion of serum from another individual. He explained that the agglutination reaction was because of interaction between RBC antigen and antibodies present in serum and developed first blood group system i.e. ABO.
I. ABO Blood Group System
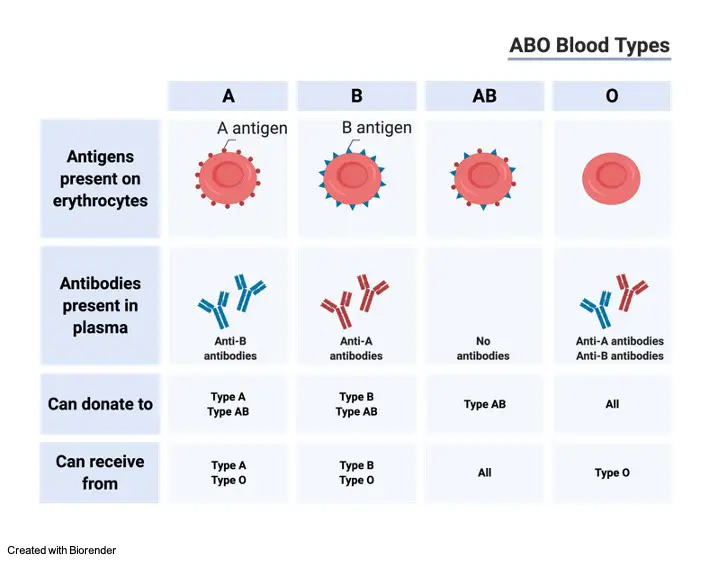
o ABO system has 4 blood groups: A, B, O, and AB
1. Blood Group A: It shows Expression antigen A on the RBC surface and antibody B in the plasma. Individuals with this blood group A can receive blood from people with blood group A and O.
2. Blood Group B: B Antigen is expressed on the RBC surface in these individuals and antibody A in the plasma. Individuals with this blood group B can receive blood from people with blood group B and O.
3. Blood Group AB: Some Individuals have both A and B antigens on the RBC surface and no antibody A and antibody B in the plasma. Individuals with this blood group AB can receive blood from people with blood group A, B and O
4. Blood Group O: Some Individuals have neither A nor B antigens on the RBC surface but have antibody A and antibody B in the plasma. These RBCs do not agglutinate with other’s plasma. Individuals with this blood group AB can receive blood from people with blood group O.
Genetics of ABO Blood Group System
o The ABO locus is present on chromosome 9, can be in any of the three allelic forms—A, B, and O. One of these alleles comes from each parent.
o Even though there are 6 genotypes (AA, BB, AB, AO, BO, and OO), they only show 4 phenotypes (blood types) because O shows no antigen.
o Some deletion on Exon 6 on this locus is found in O allele cause of loss of enzymatic activity.
o The ABO locus encodes for enzyme glycosyltransferases that are required for synthesizing A and B antigens. H antigen is a precursor for A or B antigen, this H antigen is synthesized by an enzyme which is by the FUT1 gene on the H locus.
In all blood group antigens, the ABO antigen shows most of the immunogenicity. So, the ABO system is the most important factor to be considered for transfusion and transplantation.
II. Rhesus (Rh) System
o Rhesus factor is an antigen present on RBCs. Rhesus-system has over 50 antigens and only five of them are important namely D, C, c, E, and e.
o It is the second most important blood grouping system after ABO system.
o In an individual, if a D antigen is present on the surface of RBC then it indicates that the blood group is Rh-positive and the absence of D antigen indicates Rh-negative.
o Rh antigens are encoded by highly polymorphic genes. RHD and RHCE genes (chromosome 1) are closely linked and due to high genetic rearrangements have lead production of many distinct Rh antigens.
o These 2 genes encode 400 residues long transmembrane protein.
o Between the blood types mostly there is a difference of one or two amino acids but the Rh blood group D antigen difference by 35 amino acids from the C/c and E/e antigens.
o Rh antigens are very immunogenic, e.g., if RH Negative person will produce antibody D if it comes across D Antigen which may lead to a hemolytic reaction.
III. Kell system
o It was discovered by Mrs. Kellacher. This system has 25 antigens out of which antigen k is the most clinically significant. KEL gene on chromosome 7 encodes for Kel antigen and this locus is highly polymorphic and produces many Kell antigens.
o It has the third most potent immunogenic antigens. Antibodies against Kell antigens can cause severe transfusion reactions, severe fetal anemia, and Hemolytic disease of the newborn (HDN).
IV. MNS Antigen system
o This system has a total of 42 antigens (M, N, S, and s are most common) the antigens are carried on Glycophorin A and Glycophorin B on the surface of RBCs encoded by Gene GYPA and GYPB. the antigen encoding genes are present on chromosome 4.
o One end of a glycophorin is attached to the underlying cell, and the other end has the sugar group that determines MNS blood type. Antibodies produced against it are rarely associated with transfusion reaction and HDN
V. Kidd system
o This system has 3 jk (Kidd) antigens (Jka, Jkb, JK3), it is a glycoprotein encoded by the SLC14A1 gene on chromosome 18. In RBCs, its function is to act as a urea transporter. Kidd’s antibodies are rare but tend to cause a transfusion reaction.
o Anti-Jka and anti-Jkb are difficult to detect. But the HDN by the anti-Kidd antibodies is mostly mild.
Blood Group Disorder
Hemolytic disease of the newborn (HDN) and transfusion reaction;
o Transfusion Reaction: Reaction takes place when incompatible donor blood is given to patient circulation, which evokes the Patient’s immune system. When such incompatible donor’s RBCs are destroyed by antibodies in the Patient it is called a hemolytic transfusion reaction.
o Hemolytic Disease of the Newborn: HDN is caused when the antibodies of the mother and attacks RBCs of the fetus because of the incompatibility between their blood antigen. A major cause of HDN is Rh and sometimes ABO too but ABO is found to be less severe. Hemolytic reactions against Antigens of the Kell blood group, Kidd blood group, and MNS aren’t a common cause of HDN.
Blood Grouping and Cross-matching
o Blood Grouping refers to determining blood’s ABO type and Rh D status.
o For example, a patient having blood group A can receive blood from a donor with blood group A or O but donors with blood group B or AB are incompatible.
o Sometimes donor blood can be the incompatible cause of other antigens (that are not often typed) which may cause a problem due to the presence of antibodies against it in recipient serum.
o To overcome this problem cross-matching test ensures compatibility. It ensures safe blood transfusion. In the case of incompatibility recipient’s blood can evoke the recipient’s immune system against donor cells which can lead to kidney failure, shock, and death.
Procedure
1. ABO typing is a test carried out to determine the blood group. In blood samples, anti-A and anti-B antibodies are added the sample is examined for the agglutination. Rh D typing is done similarly by Anti Rh D.
2. Next step is cross-matching which takes up to 60minutes. It is carried out by mixing a sample of Donor RBCs with the recipient’s serum to detect the reaction which is examined under the microscope, if agglutination occurs then the proposed transfusion is incompatible.
You may like to read;
Blood Cells: Definition, Composition, and Functions
Respiratory Volume and Respiratory Capacity
Digestion of Food: Definition, Mechanism, and Process
Absorption of Food: Definition, Types, and Mechanism
Human Respiratory System: Definition, Mechanism, and Facts
Krebs Cycle: Definition, Diagram, Steps, and Mechanism
Blood Group Citations
- Blood group terminology: current conventions. Transfusion . Jan-Feb 1984;24(1):2-7.
- Tissue distribution of histo-blood group antigens. APMIS . 2000 Jan;108(1):1-28.